Psoriasis is a chronic inflammatory disease with an immune base that causes characteristic reddened and flaking plaques to appear on the skin, especially on the elbows and knees, but also on the hands, arms, legs, trunk, face, and scalp. Sufferers, in addition to regularly using medication prescribed by the doctor and taking special care of the epidermis every day, can also obtain relief from symptoms through appropriate food choices. In particular, foods and drinks with anti-inflammatory activity should be preferred, while those that can promote the triggering of skin manifestations, starting with alcohol, should be avoided. Find out here which ones are .
derma
The benefits of retinoids against time
Retinoids are used to limit the effects of skin aging, in psoriasis and other dermatological conditions. They stimulate the production of collagen, the protein that keeps skin elastic. Here’s what you need to know.
The truth about suppurative hydradenitis
How many people are affected by this condition that causes pimple-like bumps on the skin? Is it contagious? What factors can make symptoms worse? Here’s what you need to know.
Milk scab (or childhood seborrheic dermatitis): what it is and what needs to be done
Seborrheic dermatitis is one of the most common skin conditions: it can resolve in the first year of life or instead have a chronic relapsing course (and thus recur over the years).
At the root of seborrheic dermatitis is an inflammation of the skin involving the areas of the body richest in pilo sebaceous glands (i.e., very small glands connected to the hair and producing a substance called sebum). This inflammation causes reddening of the skin and the formation of scales, which can be dry or yellowish and greasy.
Read more.
What is it and how does epidermolysis bullosa manifest itself?
Epidermolysis bullosa is the generic name given to a group of genetic diseases in which the skin and mucosal lining tissues (epithelia) undergo, either spontaneously or as a result of minimal trauma, dislodging and blistering. Severity varies widely: there are mild forms that allow near-normal life and very severe forms, which can be lethal in neonatal or prenatal life. The first symptoms usually occur in the first few months of life. Based on the depth of the lesions, bullous epidermolysis is divided into three classes: simple, junctional, and dystrophic. In the simple forms, the epidermis (the most superficial layer of skin) is involved, while the mucous membranes are rarely affected; boils heal without scarring, and the main complication is infection of the lesions. In the junctional forms, the lesions are deeper (between the epidermis and the dermis), and the boils are extensive and often involve the mucous membranes; lethal epidermolysis bullosa (Herlitz type) belongs to this group.
Read more.
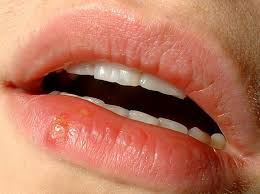
Genital herpes
Genital herpes is the most prevalent sexually transmitted ulcerative disease in developed countries. It is caused by human herpes viruses 1 (herpes simplex virus-1) or 2 (herpes simplex virus-2), which are two of the 8 types of herpesviruses that infect humans.
After initial infection, the herpes simplex virus remains dormant in nerve ganglia from which it can periodically reactivate. When the virus emerges, it may or may not cause symptoms (i.e., genital lesions). Transmission can occur through contact with lesions or, more often, through skin-to-skin contact with sexual partners when lesions are not obvious (called asymptomatic shedding).
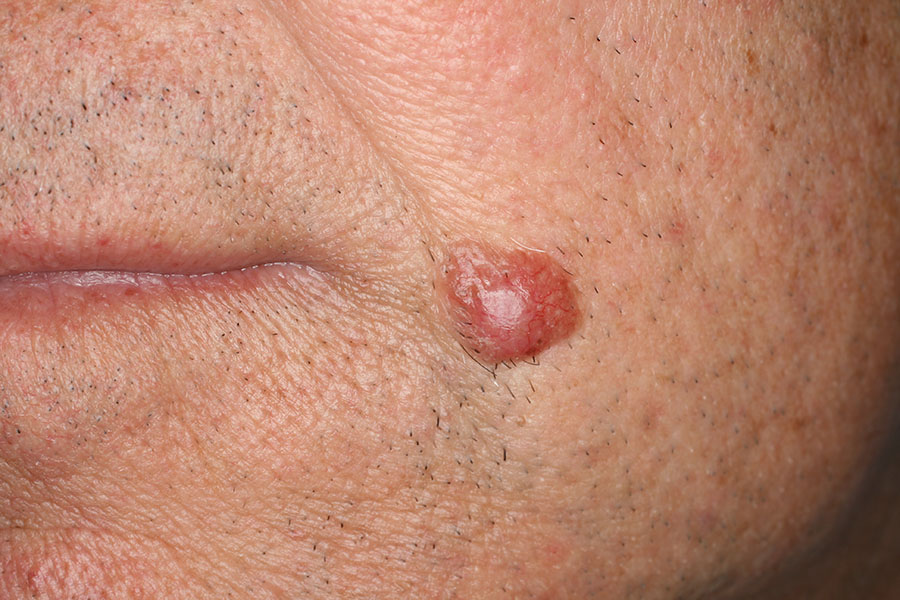
Epithelioma: causes and symptoms
Epitheliomas, although malignant tumors, rarely produce metastases. Thus, their malignancy is mainly expressed in the area of onset, and their surgical removal is almost always resolving. They are divided into Basaliomas (basal cell carcinoma) and Spinaliomas (spinocellular carcinomas).
Their occurrence is closely related to sun exposure (long and sustained) and prefers fair-skinned subjects, photo-exposed areas, and subjects who for work or play activities are exposed to the sun for a long time. Inevitably, a genetic predisposition is always present.
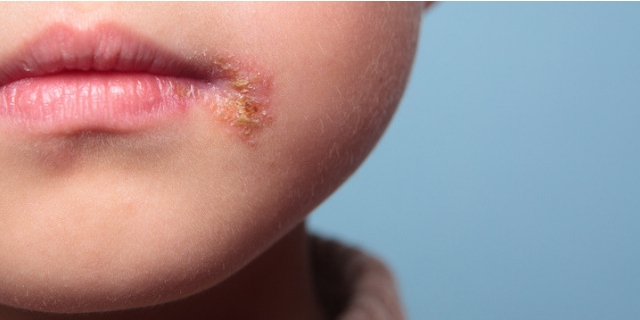
Herpes simplex virus infections
Herpes simplex viruses (human herpes virus types 1 and 2, HHV-1 and 2) commonly cause a relapsing infection affecting skin, mouth, lips, eyes, and genitalia. Common serious variants include encephalitis, meningitis, neonatal herpes, and disseminated infections in immunocompromised patients. Mucocutaneous infections manifest as clusters of small, painful, erythematous-based blisters. Diagnosis is clinical; laboratory confirmation can be obtained through culture tests, PCR (polymerase chain reaction), direct immunofluorescence, or serologic tests. Therapy is symptomatic; antiviral treatment with acyclovir, valacyclovir, or famciclovir is useful in severe infections and, if started early, in primary or recurrent infections.
Mycosis: the fungi of the skin
Mycoses are infections generated by fungi that, like bacteria, can reproduce in the human body.
Specifically addressed below are the benign type forms, which, often, do not present any symptoms and are more frequent in the summer period. For this reason, we will try to clarify well:
– What are mycoses and who are those most at risk?
– How and where can mycoses be contracted?
– Treating mycosis: how to intervene?
What are mycoses and who are those most at risk?
Mycoses are infections that can affect the skin, hair, nails, and mucous membranes, and can be classified into the following categories:
- Superficial, that is, mycoses affecting the skin, scalp, or nails
- Subcutaneous, which are more invasive infections that penetrate within the dermis and subcutaneous tissues
- Systemic, that is, mycoses that affect internal organs or the blood, and, therefore, very dangerous
- Opportunistic, which are infections that can be very serious and mainly affect people with immune system deficiencies
Mycoses can be, therefore, also very serious, invading mucous membranes and internal organs. They particularly occur in patients with reduced immunological defenses, such as in organ transplant recipients or patients undergoing chemotherapy. Chemotherapeutics decrease white blood cells, which are an initial barrier against the invasion of microorganisms, including fungi. Cortisone treatments in particular can promote fungal infections.
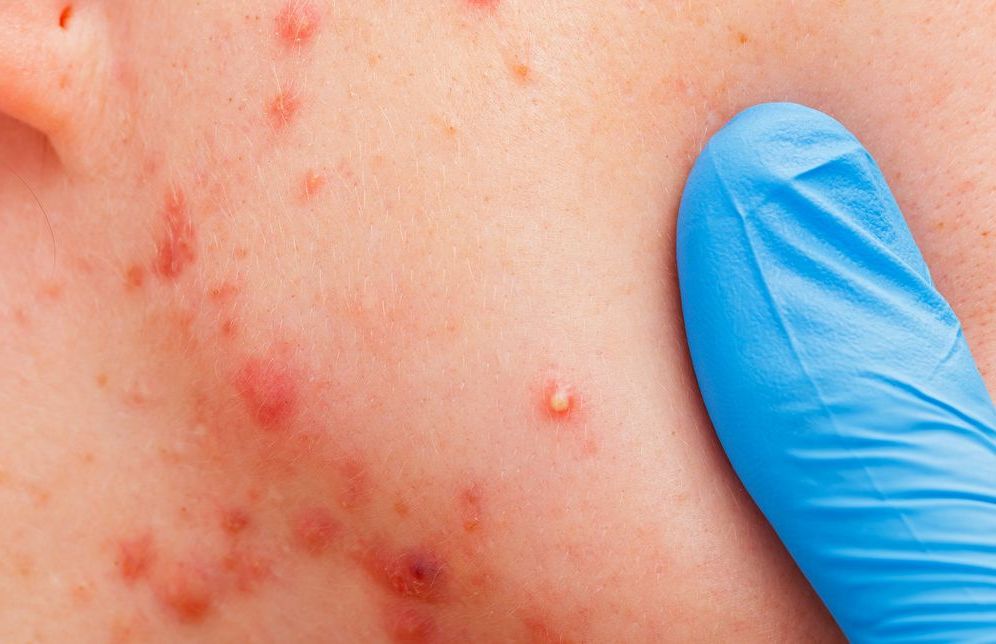
Furunculosis – What is it?
Furunculosis is a deep infection of hair follicles generally caused by the bacterium Staphylococcus aureus and mainly affecting the face.
Furunculosis is a deep infection of hair follicles generally caused by the bacterium Staphylococcus aureus And mainly affecting the face. I furuncles, which can occur either singly or in groups, present as a raised, reddened lesion with a hard, painful nodular central part; over time, the furuncles may enlarge and pus formation may occur at the top of them.
Furuncles can form due to excess production of sebum by the sebaceous glands of the epidermis (due to genetic or hormonal reasons), such that they clog the pores of the skin and interact with the resident microbial microflora: thus an inflammatory reaction is generated, resulting in lesion formation. In some cases, however, the formation of furuncles may be related to the presence of an ingrown hair or foreign body in the hair follicle.
Gonorrhea: what is it
Gonorrhea is caused by the bacterium Neisseria gonorrhoeae. Gonorrhea is caused by the bacterium Neisseria gonorrhoeae, which characteristically infects the epithelium of the bladder, cervix, rectum, pharynx, or conjunctiva, and causes inflammation and purulent discharge. Spread to the skin and joints, which is not uncommon, causes skin wounds, fever, and migrating polyarthritis or pauciarticular septic arthritis. Diagnosis is made under the microscope, by culture examination or by nucleic acid amplification tests. Many oral or injectable antibiotics can be used; however, drug resistance is a growing problem.
Kaposi’s disease: what is it?
Kaposi’s sarcoma is a rare type of cancer caused by a virus, called HHV8, belonging to the herpes virus family. It can affect both the skin and internal organs.
Approximately 30-40% of patients with human immunodeficiency virus (HIV) infection who are not treated with so-called antiretroviral drugs are likely to develop Kaposi’s sarcoma and/or lymphomas during the course of the disease. Kaposi’s sarcoma can also occur in people with weakened immune systems or a genetic predisposition.
In industrialized countries, it is 2000 times more common in people with HIV than in the general population. In the United States of America (USA) and Europe, the prevalence (prevalence) of Kaposi’s sarcoma, in men with AIDS, varies from 1% in hemophiliacs to 21% in homosexuals, if they are not treated with the now widely available HIV therapies.
Cutaneous angioma
Skin angiomas are mostly benign neoformations due to the abnormal cellular development of sanguneous or lymphatic vessels. The most common form of cutaneous angioma is hemangioma, which consists of a proliferation of blood vessels and usually appears at birth or during the first year of life, then recedes spontaneously over time, requiring no treatment. Much rarer is lymphangioma, which affects lymphatic vessels and can be capillary or cystic in nature.
Syphilis: what you need to know
Syphilis is a sexually transmitted infection (STI) caused by the bacterium Treponema pallidum. Globally, it is the third most common bacterial-type HIST after chlamydia and gonorrhea.
Transmission
Syphilis is transmitted through any type of sexual intercourse (vaginal, anal and oral) and by blood. An infected mother can transmit syphilis to her unborn child during pregnancy (transplacental route), through passage through the birth canal, and by breastfeeding.
Specifically, it is defined as:
- Acquired syphilis the infection contracted after birth
- Congenital or prenatal syphilis that contracted transplacentally
- Connatal syphilis that acquired at the time of passage through the birth canal.
Warts: what are they?
Warts are skin lesions that, depending on their location, can be distinguished into vulgar warts, when present on the body, and genital warts.
In general, vulgar warts affect the face, including the oral and nasal mucosa, hands, and feet. Genital warts, which are due to different viral strains, are also known as condylomata, and are mostly observed on the genital and perianal region, although it is not excluded that verrucas of the vulgar type may also occur in this area.
Vitiligo
- Areas of lightened skin are found on various parts of the body.
- In general, doctors base their diagnosis on the appearance of the skin.
- Corticosteroid creams, other medications or phototherapy in addition to light-sensitizing drugs can help repigment the skin, or skin grafts can be used if necessary.
Up to 2% of the population suffers from vitiligo.
The cause of vitiligo is unknown, but it is a skin pigmentation disorder that may involve an attack by the immune system on the cells that produce the skin pigment melanin (melanocytes). Vitiligo may run in families or may develop spontaneously. It may occur in conjunction with certain other diseases, and is associated with autoimmune diseases (when the body attacks its own tissues), of which thyroid diseases are the most common. It is most closely associated with diseases that make the thyroid overactive and those that make the thyroid hypoactive . People with diabetes, Addison’s disease, and pernicious anemia are also more likely to have vitiligo. However, the relationship between these disorders and vitiligo is unclear.