Diabetes is a metabolic disease related to the body’s inability to produce or properly use insulin. In the first case, it is called type 1 diabetes (rarer), and in the second case, it is called type 2 diabetes (more common in adults). The video explains why the two forms occur and why a healthy lifestyle is important to prevent and slow their progression.
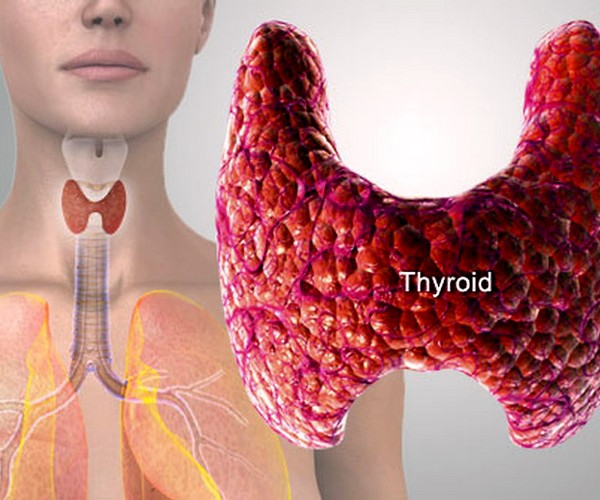
“Diabetes” refers to a group of conditions characterized by high blood glucose levels, commonly known as blood sugar. Glucose comes from the digestion of carbohydrates found in food and is transported by the bloodstream to various tissues in the body. However, glucose cannot pass through the cell membrane and enter the cells on its own; it needs the help of a hormone produced by the pancreas called insulin.
When insulin binds to its receptor on target cells, it triggers a signaling cascade that exposes glucose transporters on the cell membrane, creating openings that allow glucose to enter the cells. In most tissues, such as muscles, glucose is used as an energy source, while in the liver and adipose tissue, it is also stored for later use, in the form of glycogen and fats.
When the body is in a fasting state, the liver produces and secretes glucose into the bloodstream, while adipose tissue releases free fatty acids and sends them to the liver, where they are converted into additional metabolic energy. Diabetes occurs when there is insufficient insulin or when its action is compromised. Without insulin, glucose cannot enter the cells; it remains in the blood, causing hyperglycemia.
There are two main types of diabetes. Type 1 occurs when the pancreas does not produce enough insulin; type 2 occurs when the body’s cells do not respond well to insulin because they are “insulin-resistant.” Both types are caused by a combination of genetic and environmental factors, but genetics plays a dominant role in type 1, while lifestyle is a predominant risk factor in type 2.
For this reason, type 1 diabetes usually develops suddenly in childhood, while type 2 progresses gradually during adulthood, passing through the so-called pre-diabetic state, which is defined as having borderline blood sugar levels: higher than normal but lower than typical for diabetes. Pre-diabetes is very common and, although it does not always develop into full-blown diabetes, over time it can cause similar damage to the body. An unhealthy lifestyle is the trigger for pre-diabetes and the main driver of its progression to type 2 diabetes. Key factors include obesity and physical inactivity.
There are at least two ways in which obesity can lead to insulin resistance and hyperglycemia.
First, in obesity, fat cells are forced to process more nutrients than they can handle and become stressed. As a result, they begin to release inflammatory mediators known as cytokines. Cytokines interfere with the insulin receptor signaling cascade, blocking the action of insulin and making the cells less responsive to it.
Second, excess adipose tissue releases and sends excessive amounts of free fatty acids to the liver – an event that normally only occurs during fasting. This causes the liver to produce and release more glucose into the blood. Hyperglycemia stimulates further insulin secretion. Constantly high insulin levels desensitize the tissues, causing insulin resistance.
Abdominal fat seems to produce more fatty acids and cytokines, and thus has a more severe effect on blood sugar levels than subcutaneous or peripheral fat. For this reason, an excessive waist circumference is a more significant risk factor than body mass index (BMI).
A sedentary lifestyle, in addition to indirectly causing weight gain, directly impacts insulin resistance. This happens because physical activity is necessary to maintain “healthy” blood sugar levels. Physical activity increases the energy demand of muscles, which consume glucose from the blood and later glucose stored in the liver and adipose tissue.
A high energy expenditure helps normalize blood sugar spikes that follow meals more quickly. Additionally, high energy demand promotes a better cellular response to insulin, increasing insulin sensitivity. Studies have shown that physical inactivity, even for a short period, results in significantly higher blood sugar spikes after meals, which can lead to pre-diabetic changes in healthy individuals or accelerate the transition from pre-diabetes to full-blown diabetes.
It is important to note that this does not only occur in overweight patients, but also in individuals with a seemingly “healthy” weight. This likely happens because inactivity reduces muscle mass and replaces it with adipose tissue, which has serious effects on blood sugar levels even if overall weight remains within normal limits.
The key concept is that, to prevent diabetes, weight control must be combined with physical activity or exercise.
Source: Alila Medical Media