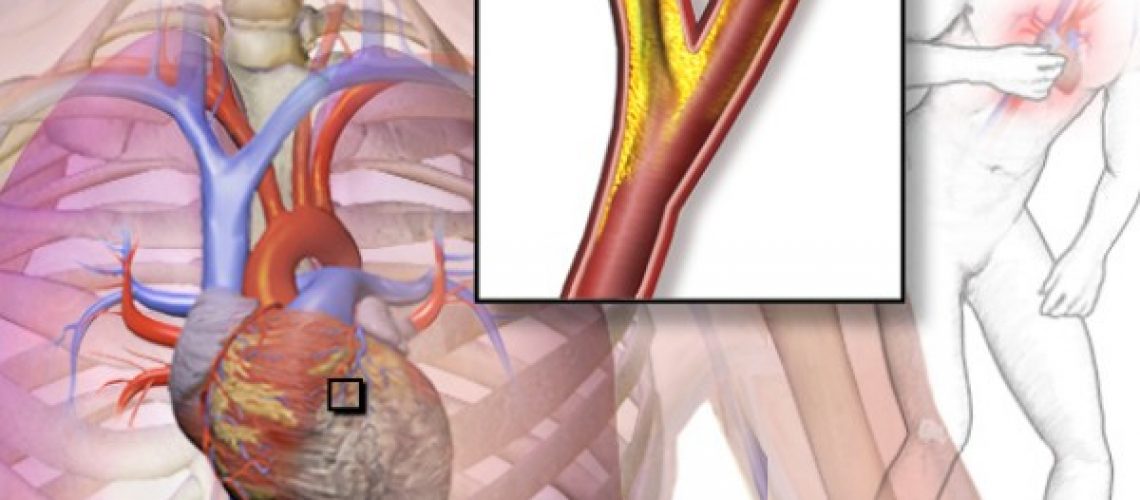
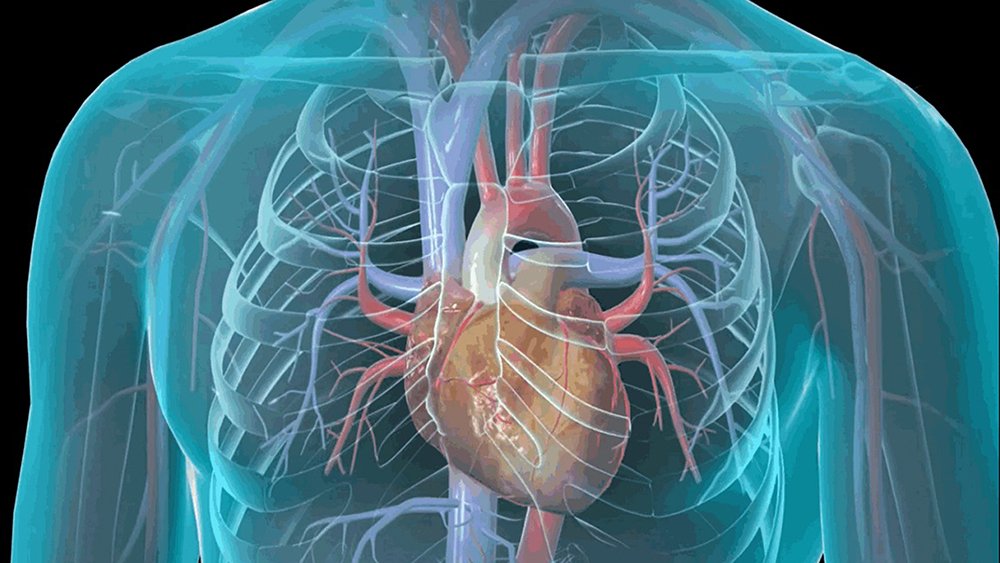
Referred to by the Latin name for its main manifestation, a weight-like or vice-like tightness in the chest, angina pectoris is not a disease per se, but the consequence of changes in the coronary arteries that prevent these arteries from providing an adequate and constant blood supply to the entire heart muscle.
There are four types of angina, differing in characteristics, etiopathogenesis, and severity: chronic stable, unstable, vasospastic/variant (also called Prinzmetal’s angina), and microvascular.
Angina is defined as “stable” when the onset of symptoms is predictable: it is the most common and easiest form to keep under control and is caused by narrowing of the coronary arteries associated with atherosclerotic pathology, or the deposition of cholesterol plaques along the inner walls of the arteries.
Unstable angina is more problematic to manage because attacks arise unpredictably, often even after minimal exertion or even at rest, due to psychoemotional stress or during sleep, causing abrupt awakenings. This form of angina is also called pre-infarct angina because it represents a kind of “antechamber” to heart attack and, if not treated properly, can be life-threatening.
Vasospastic/variant angina is characterized by pain that occurs at rest and disappears on its own after a few minutes, whereas microvascular angina mainly affects women and manifests itself with similar characteristics to chronic stable angina but with attacks of longer duration.