“M” for meningococcal meningitis.
What is meant by meningitis?
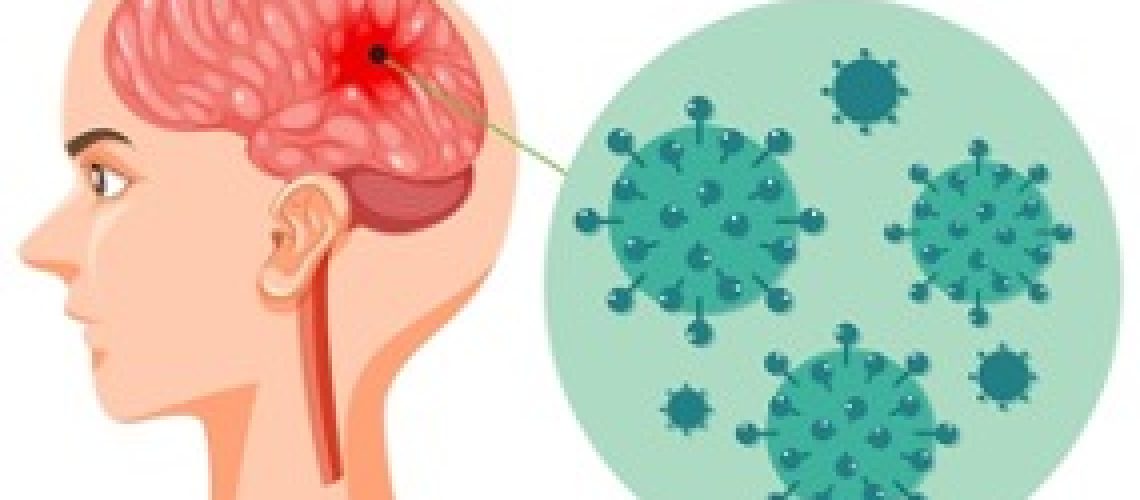
Although the term immediately evokes the meningococcal form, it should not be forgotten that “meningitis” means inflammation of the meninges, that is, the envelope, consisting of three leaflets, that lines the central nervous system. The meninges can also be affected by other microbial agents, either bacterial (e.g., pneumococcal, hemophilic) or viral or fungal, and also involved in traumatic events.

Why is meningitis so scary?
The practice conveys two important experiences or, if you prefer, two messages: first, it is more likely to be feared than a danger that one touches with one’s hands or that, even without seeing, one can sense or even imagine; second, it is difficult to place a value on prevention: if the majority of the population or at-risk individuals vaccinate, the expected effect is the absence (or near absence) of disease. But if this goal is achieved, it is not a foregone conclusion! If the strategies work, in fact, the problem does not emerge, and only a statistical estimate will be able to speculate how many cases have been avoided.
What characterizes bacterial (meningococcal) meningitis?
With regard to bacterial meningitis, what is most striking and frightening is its impact, which could be described as rapid and devastating: it affects healthy individuals of all ages, manifests insidiously, and leaves little time margin for intervention. This is due both to the behavior of perhaps the best known microorganism, meningococcus, and to the fact that the target is the nervous system, by far the most vulnerable organ. Not only that. Although there are fewer cases of meningitis each year than deaths from traffic accidents-and the figures have remained stable in recent years, so there is no justification for thinking of a health or social alarm-one in ten children goes on to die and more than one in three to suffer permanent and disabling consequences, including sensory neurological deficits (e.g., deafness, blindness), motor and cognitive impairments.ù

Who is most at risk?
Those most susceptible to bacterial meningitis are infants (by the way, in the first year of life, hemophilus and pneumococcus are also relevant among the causes in addition to meningococcus), followed by adolescents. All age groups, however, should be considered at risk: cases have occurred in young people returning from a party, teachers, adults traveling to countries with high infection rates, and so on. However, there is a common denominator: close contact. Meningococcus, in fact, is transmitted if two individuals stand a few tens of centimeters apart, which explains why schools, oratories, gyms, discos, movie theaters and offices are the places where infection is most likely to occur.

Can home insulation be a prevention strategy?
No! Where then did the meningococcus come from? Simple, from healthy carriers. About one in ten individuals unknowingly harbor it in their nasal passages. It is unclear why a germ in seemingly quiet conditions becomes active and gives rise to disease. Of the 13 different types of meningococcus that exist, only five (A, B, C, W135 and Y, of which B and C are the most common in Europe) cause meningitis and other serious illnesses. And specific vaccines are available against them, which among other things have been included in the current Vaccine Plan. Vaccination against meningococcal B is free for children during the 1st year of life: there are 3 doses at the 3rd, 4th, 6th month of life and 1 booster at the 13th month. Meningococcal C vaccination is free for children who have reached one year of age: the National Plan calls for a single administration between 13 and 15 months of age. Vaccination with tetravalent conjugate vaccine, against meningococcal A, C, W, Y, is free for adolescents: either as a booster for those who were already vaccinated against meningococcal C as children or for those who have never been vaccinated before.
Edited by Dr.Piercarlo Salari
Pediatrician and Scientific Disclosure