Roasted, salted or sugar-coated, everyone likes peanuts, but they are also one of the foods at greatest risk of triggering allergies. This is no small problem, since, often “hidden” or in trace amounts, they are contained in many industrially produced foods. A group of American allergologists has identified a simple way to make them tolerable by the immune system and avoid unpleasant episodes.
food
Vinegar of a thousand virtues: true or alleged?
Wine, red or white, balsamic, apple, pear, rice, coconut, honey or beer. These are just a few variants of vinegar much-loved food in all parts of the world and used for many different purposes. Seasoning, flavoring, cooking, preserving, disinfecting, and even achieving specific health benefits, from weight control to blood sugar control. But what is true among the many touted virtues?
Here is what is known
about this valuable fermentation product and what, on the other hand, remains to be proven.
Raw milk and dairy products: a risky fad
Eat foods as nature creates, without processing them in any way or cooking them, to benefit from all the macro- and micronutrients they contain and take advantage of their valuable properties. Put like that, that of the “crudists” sounds like an extremely healthy approach. But, in fact, it can prove dangerous to health, because heat serves to break down the bacterial load of foods (especially fresh, moist foods that are rich in protein and sugar, which are much loved by pathogenic microorganisms) and prevent food toxins. “Raw,” i.e., non-pasteurized, milk is a case in point. As demonstrated by
a recent incident in the United States
.
Doctor-prescribed fruits and vegetables? Surprising savings for the health care system
Healthy foods prescribed as if they were drugs: a new study published in March in PLoS Medicine suggests adopting this strategy in the United States for beneficiaries of Medicare and Medicaid-the two major federal health insurance programs-with the stated aim of reducing the risk of chronic diseases, such as cardiovascular disease or diabetes, while lowering the cost of care.
Making use of computer models, researchers at Tufts University in Boston estimated that healthy food prescriptions could prevent millions of cardiovascular events, such as heart attacks and strokes, and save billions of dollars in health care costs.
To run the simulations, the authors included people between the ages of 35 and 80 years and enrolled in Medicare or Medicaid; as part of the modeling, they used data from the three most recent surveys on the health and nutrition of U.S. citizens, as well as those produced by published studies in the literature and meta-analyses that included demographic information, dietary habits, and health care costs.
Several hypotheses were examined in the study: including an estimate of the impact that a 30 percent discount for purchasing doctor-prescribed healthy foods might have.
Already limiting prescriptions to
fruits and vegetables,
now consumed in insufficient quantities in the U.S., it has been estimated that 1.93 million cardiovascular events could be avoided, with a total savings of $39.7 billion. When they ran the estimate assuming a wider prescription of healthy foods, they calculated that 3.28 million cardiovascular events and 120,000 cases of diabetes would be prevented and $100.2 billion would be saved.
“We found that partial coverage of the cost of purchasing fruits, vegetables, whole grains, nuts, seeds and vegetable oils would be highly cost-effective, ” said Yujin Lee, first author of the study. and would be quite similar in cost-effectiveness to prescription drugs for high cholesterol or hypertension.”
Lee Y, Mozaffarian D, Sy S, Huang Y, Liu J, Wilde PE, Abrahams-Gessel S, Jardim TSV, Gaziano TA, Micha R. Cost-effectiveness of financial incentives for improving diet and health through Medicare and Medicaid: A microsimulation study. PLoS Med. 2019 Mar 19;16(3):e1002761.
Fighting anxiety at the table, in a healthy way
No, it is not about drowning worries about the future in food , nor is it about compensating for past stresses and frustrations with refined sugars and saturated fats, although this is the most immediate and widespread tendency. The food we choose and the way we eat them can be harnessed in a more positive way, to prevent and quell excessive nervousness and agitation, make us feel better, more relaxed, and more likely to rest well during the night (resulting in additional benefits for mood and psychophysical reactivity). Certain substances in foods, in fact, act at the brain level and if taken in the right dose, regularly or as needed, can have a positive impact on neuropsychic function.
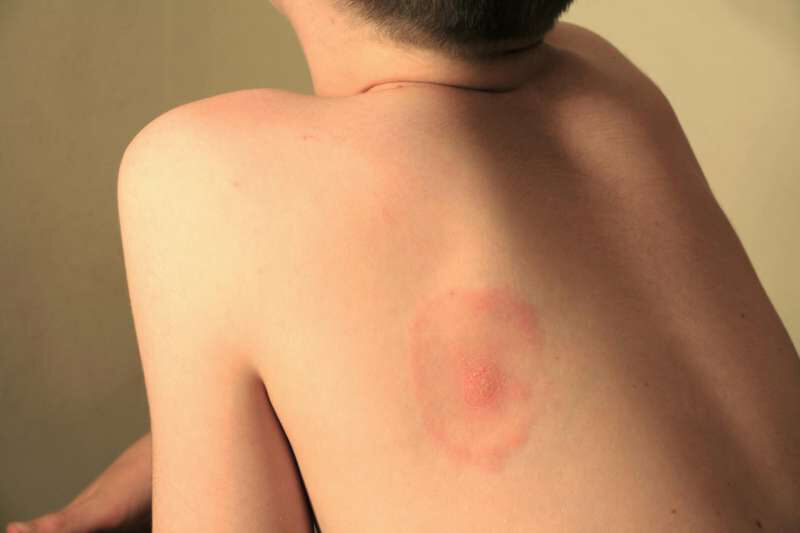
Rubbing the skin increases the risk of food allergies
Logic would dictate that what triggers food allergies. was the simple ingestion of a food containing substances (usually, proteins, peptides or particular sugars) toward which the individual immune system reacts abnormally, recognizing them as potentially dangerous and activating a whole series of defense mechanisms to try to eliminate them from the body or, at least, to neutralize their action (in fact, in itself completely harmless).
In fact, when a food to which one is allergic is ingested, the immune system initiates reactive processes such as the synthesis of histamine (on which depend the onset of oozing, red patches, rashes of various types, swelling and itching in various parts of the body) and the production of immunoglobulin E (IgE, which trigger and sustain the allergic response in various organs and tissues), to the point of triggering, in the most severe cases (fortunately rare), an anaphylactic reaction, characterized by skin reactions, bronchoconstriction, angioedema (especially in the face and throat), hypotension, and anaphylactic shock with possible onset of coma, sometimes fatal.
A study recently conducted in animal models (specifically, mice) has, however, indicated thatfood allergy could be linked to or, at the very least, be made more likely not only by the ingestion of certain foods, but also by stresses on the skin, such as those typical of scratching.
In particular, it has been observed that by mimicking scratching through the application and tearing of patches from the skin of mice, it is possible to trigger/increase intestinal reactivity to food allergens on the part of the animals, making them more likely to go through the typical symptoms already mentioned after ingesting food that is in itself completely harmless.
At the origin of this effect there would be a molecular link between the skin and the intestinal epithelium: repeated skin rubbing would trigger the release of a substance called interleukin 33 (IL-33), which, together with IL-25 produced by particular cells of the intestinal epithelium (tuft cells or “tuft cells”), would go on to stimulate a subset of immune system cells called innate lymphoid cell type 2 (ILC2) cells. The latter, through the release of IL-4, would stimulate other cells of the immune system called mast cells, which, in turn, would release mediators capable of increasing intestinal permeability to food allergens and, therefore, their absorption, resulting in an increased risk of leading to systemic allergic reactions and anaphylaxis.
If this initial evidence is confirmed in humans, the newly identified allergic communication and elicitation mechanism could explain why those with atopic dermatitis (a condition associated with skin discomfort and a tendency to repeated scratching) are more likely to also develop food allergies.
Source
J-M Leyva-Castillo, C Galand, et al. Mechanical skin injury promotes food anaphylaxis by driving intestinal mast cell expansion. Immunity 2019; doi:10.1016/j.immuni.2019.03.023 (https://www.cell.com/immunity/fulltext/S1074-7613(19)30140-2)
Liver-friendly foods
Alcoholic drinks, fried foods, sausages, fatty meats and cheeses, creams, Various sauces and gravies can be very attractive and pleasing to the palate, but they are much less so for the liver, which has to work hard to digest them. This is well known. Less well known is that there are also foods that can help the work of the liver, promoting good digestion and general well-being without sacrificing the taste. Know them, take them in the right amount every day, and maintain meal times and regular life rhythms allows one to feel fitter and avoid abdominal discomfort, headaches, fatigue and toxin accumulation harmful.
Artificial sweeteners: the position of US pediatricians
As Italy prepares to introduce the “Sugar tax,” not only to balance the state budget but also with a view to discouraging the intake of beverages (and foods) containing excess sugar and calories, U.S. pediatricians are wondering about the possible health effects of the growing number of artificial sweeteners used as substitutes by the food industry and consumed in increasing quantities by children. Consumption of which, often, parents are not fully aware, since sweeteners are listed by law only in the list of ingredients (which not everyone reads and in any case written in microscopic characters), while the “reduced sugar content” that everyone likes is always made explicit in clear letters on the packaging and in advertising claims, leading to an interpretation, if not fallacious, at least partial and somewhat distorted of the characteristics of the product being purchased.
But is there really anything to fear when it comes to artificial sweeteners approved for food use by the Regulatory Agencies (i.e. the Food and Drug Administration – FDA in the United States and theEuropean Food Security Agency – EFSA in Europe) responsible for ensuring the safety and wholesomeness of substances used to produce food of any kind? In principle, no, because only compounds for which no indications of possible harm to the human body have emerged are allowed for food use. But it is precisely on this point that theAmerican Academy of Pediatrics – AAP does not agree much and would like a little more caution from everyone, institutions, manufacturers and parents. According to the Position statement published on this matter in the scientific journal Pediatrics, in fact, while for some sweeteners that have been in use for a longer time (saccharin, aspartame, acesulfame, sucralose) health criticalities from moderate consumption can be reasonably ruled out, for others of more recent introduction (such as stevia) the evidence supporting their total harmlessness is considered insufficient, especially with regard to the effects from prolonged use and especially in children.
Not only that. One aspect that the JPA believes should be investigated further concerns quantities because, as is known, any substance can result in extremely different effects in the human body depending on how much is taken in a single day and repeatedly on successive days for varying periods of time. This is also true of common sugar, which is a harmless and valuable source of ready-to-use energy for the muscles and brain when taken in low doses, but becomes an enemy of metabolic and cardiovascular health when consumed in excessive amounts, promoting-as is well known-conditions of overweight/obesity, insulin resistance and diabetes. Unfortunately, unlike other nutrients in foods, artificial sweeteners are not required to be labeled with quantities (absolute or percentage) per 100 grams or per serving of product, which prevents (the consumer and those who have to assess individual/population exposure levels) from knowing how much they are taking in through their usual diet.
Add to this that, contrary to what was initially assumed and touted, studies to date have indicated that consumption of artificial sweeteners in place of common sugar is not necessarily associated with weight loss unless their use is part of an overall healthy, balanced diet aimed at weight loss. Thus, opting for “low-sugar” or “zero-sugar” beverages or foods, per se, does not help counter the growing prevalence of overweight and obesity, either among adults or children.
Given these considerations, while not wishing to generate unreasonable alarmism, U.S. pediatricians believe that more in-depth studies need to be conducted to assess the long-term effects of different artificial sweeteners, including on children’s intake levels, and which parents should be better informed about the properties and, more importantly, the amounts of artificial sweeteners in commercially available industrial food products to support informed choices and avoid excessive intakes.
Source:
CM Baker-Smith et al. The Use of Nonnutritive sweeteners in Children – American Academy of Pediatrics (AAP) Policy Statement. Pediatrics 2019;114(5):e20192765; doi:10.1542/peds.2019-2765(www.aap.org/en-us/about-the-aap/aap-press-room/Pages/American-Academy-of-Pediatrics-Looks-at-Use-of-Nonnutritive-Sweeteners-by-Children.aspx; pediatrics.aappublications.org/content/early/2019/10/25/peds.2019-2765)