Ultrasound is a diagnostic imaging technique based on the use of ultrasound that is quick and easy to perform, harmless, painless, and low-cost, and because of these favorable characteristics it has become extremely popular over the past 30 years in countless clinical settings.
Currently, there are many variants of ultrasound investigation that improve its resolution and information power according to its applications (conventional external, color, transvaginal, transrectal, transesophageal).
The main limitation of the method lies in the fact that it is “operator-dependent”: meaning that its diagnostic usefulness is tied to the experience and ability of the physician performing it to interpret the ultrasound images obtained.
Description
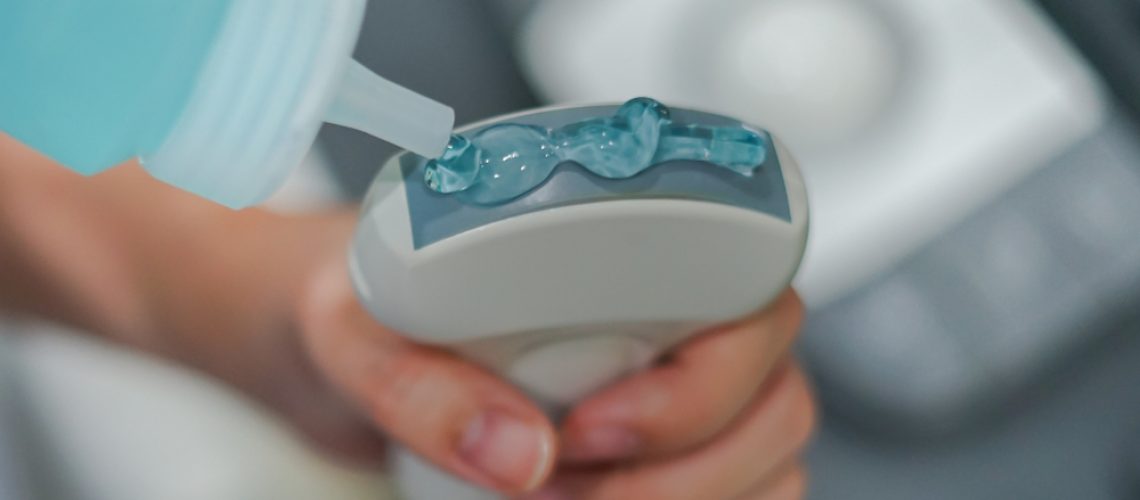
Generally, conventional ultrasound is performed from the outside, resting the ultrasound scanner’s sensor/transducer (similar to a microphone or joystick) on clean, dry skin, previously covered with a special transparent gel that makes it possible to improve the transmission of signals from the inside of the body to the sensor and vice versa, making it more homogeneous by eliminating air bubbles.
The sensor/transducer sends diagnostic ultrasound (completely harmless), which passes through the body tissues for a few centimeters and is partially “reflected” by them back to the sensor/transducer, differentially depending on the characteristics of the tissue itself. The signals received and transduced by the sensor into electrical pulses are sent to the ultrasound scanner, which translates them into images (black and white or color), displayed on the monitor in real time.
This makes it possible not only to visualize all the structures in the area scanned by the ultrasound scanner, but also to assess their dynamic relationships related to the physiological movement of different organs.
Generally, the physician focuses attention on specific tissues or structures, based on the clinical rationale for requesting the ultrasound, and in the course of the examination takes snapshots of images on the monitor that he or she considers to be of particular relevance for diagnostic purposes. At the end of the examination, which on average takes about 15 to 20 minutes (depending on the extent of the area to be evaluated, the quality of the images obtained, and the clinical situation), simply remove the gel with paper towels and dress. The report is usually delivered immediately.
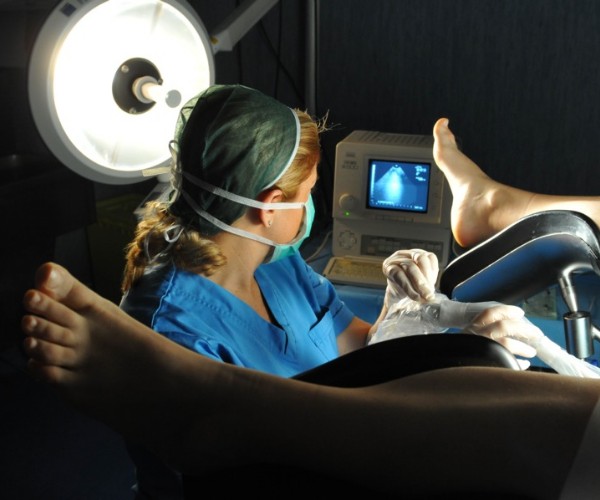
In the gynecologic setting, ultrasound can be performed externally (as is the case with ultrasound scans performed during pregnancy) or endovaginally (a modality commonly used during gynecologic checkups to better visualize the uterus, fallopian tubes, and ovaries.
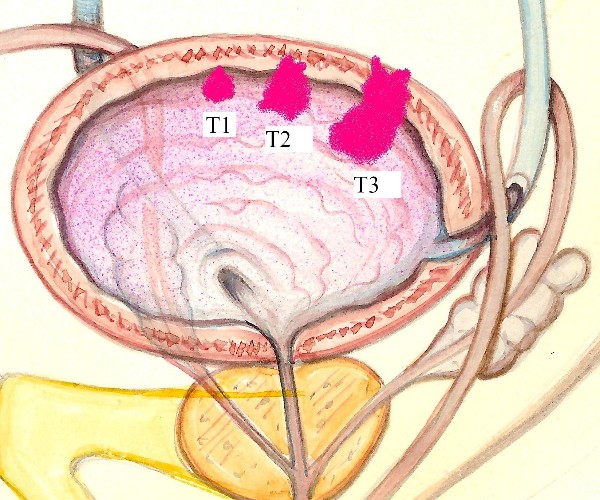
In urology, ultrasound can be performed externally (for example, to assess the status of the kidneys) or transrectally (a modality used to investigate the prostate).
The transesophageal variant, on the other hand, is used in cardiology to obtain images of the heart in motion. In this case, the examination is called an echocardiogram, and its execution involves preliminary sedation to facilitate the introduction of the tube with the sensor/transducer placed at the end.
When needed
Ultrasound can be performed to assess the status of virtually all soft tissues and the morphology, movement, and dynamic relationships between neighboring organs.
The most common indications of ultrasound include:
- evaluation of the gallbladder (to highlight stones) and liver (to assess its enlargement, presence of fibrosis or abnormal formations, etc.);
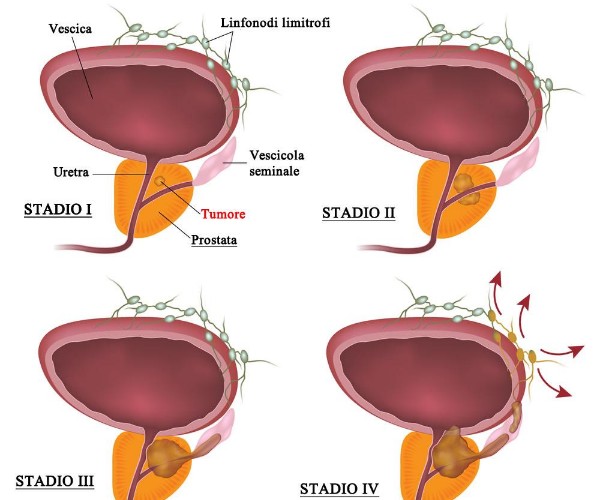
- evaluation of the status of the kidneys (to locate stones, cysts or other abnormal formations), bladder and prostate in men (size, presence of abnormal formations, etc.);
- Fetal monitoring during periodic checkups during pregnancy;
- evaluation of the status of the uterus, fallopian tubes, and ovaries as part of routine gynecological checkups or aimed at diagnosing/monitoring specific diseases;
- Diagnosis and monitoring of breast cancer;
- Assessment of the size, structure, and dynamic function of the heart, heart valves, and related vessels;
- investigation of the thyroid gland aimed at examining its size, glandular tissue status, and the presence of tumors;
- investigation of the salivary glands aimed at examining their size, glandular tissue status, and the presence of stones or tumors;
- Examination of joint soft tissues (joint capsules, menisci, tendons, ligaments, etc.).
Special Warnings
Depending on the part of the body to be examined and the rules provided by the individual Clinical Center, the performance of ultrasound may or may not involve preliminary preparation.
For example, in the case of full abdomen ultrasound, it is, as a rule, necessary to observe fasting for 6-8 hours and to present with a full bladder at the time of the examination, while in the case of transvaginal ultrasound, the period of menstrual flow should be avoided. In the case of ultrasound scans of the neck (thyroid, salivary glands) or joints, however, no special preparation is required.
Generally, all the information needed to arrive in ideal condition at the time of the test is communicated (verbally and in writing) when the appointment is made: it is good to remember it and to implement what is recommended to avoid not being able to perform the test on the scheduled day and time or getting unreliable diagnostic outcomes.